There are many reasons why women choose or are required to undergo Breast Implant Revision Surgery.
It may be due to medical reasons, the implants may feel too large or too small, or it may be that body changes from pregnancy, weight fluctuations and natural ageing has left you unhappy with the current appearance of your breasts. Or it may be simply that a change in lifestyle means you no longer want to have breast implants. Whatever your reasons are for wanting breast implant revision surgery, it is important to consult an experienced plastic surgeon who can discuss all your options with you so you can make an informed decision.
As with any type of surgery, there are complications that may occur following a Breast augmentation or Breast Implant Surgery. It’s very important, that when considering breast augmentation surgery, you discuss these possible complications with your surgeon. Whilst some issues that lead to occurrence of these complications can be beyond the control of you or your surgeon, the risks can be reduced if you choose a skilled and experienced surgeon who prioritises your wellbeing rather than agreeing with everything you ask for even though he knows that this would cause issues for you in the future.
Many times correct and suitable implant selection based on patient’s height, width of shoulders and hips, chest anatomy and measurements, thickness of breast tissue will minimise the risks. Another important factor that will reduce the risk, is to carefully follow your surgeon’s pre and post-surgery instructions.
Prevention is always better than Cure…
In this article, Mr Allen Rezai, Consultant Plastic, Aesthetic & Reconstructive Surgeon, shares information regarding some known implant related complications that may lead to the need of breast implant revision surgery. It should be noted that most of these complications are very rare, especially if you choose an experienced plastic surgeon. But nevertheless, it is important for you to know and understand all the possible risks and complications involved, how these can be prevented, or the risk minimised and what treatment options are available if you experience any of these complications.
This will not take place of a ONE to ONE consultation; nevertheless, it can be useful. Remember, Knowledge is Power, and you should make sure you know all aspects of a procedure before you commit.
One Last Word Of Advice

It should be noted that secondary surgery is always more difficult than primary breast augmentation, for several reasons. First, the presence of scar tissue makes it more difficult to predict a good result. In addition, the surgeon is dealing with the stretching of tissues or anatomical changes caused by previous implants.
As it is with everything in Life, “Prevention as Always Better than a Cure”. But sometimes you can have the BEST and MOST EXPERIENCED surgeon treating you and you take all the necessary precautions, yet, complications can still occur, it’s not in your fault or your surgeons, and what is important at this stage is how it is dealt with and treated.
To conclude, we asked Mr Allen Rezai to provide a list of what he believes to be the most important considerations to be taken into account when contemplating Breast Surgery and choosing a surgeon. The following was his reply in the form of a simple but comprehensive checklist:
At Allen Rezai MD, All Procedures Are Tailored To Your Needs.


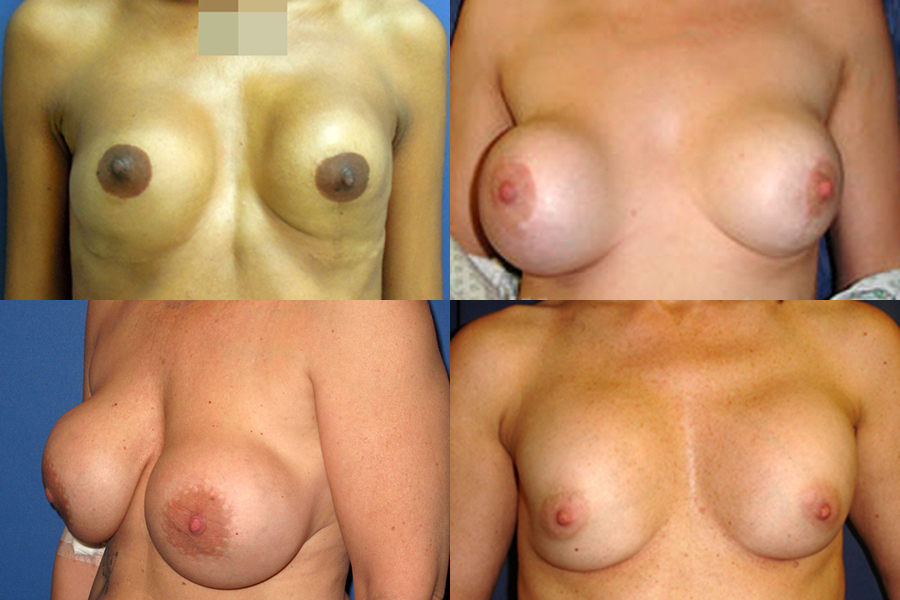 Once the breast implant is in place, as normal part of the healing process, the body forms a tissue capsule (aka barrier of scar tissue) around the implant. The body forms a capsule like this around any object it recognises as foreign as a protective measure. The tissue capsule around the implant is usually soft or slightly firm but not noticeable, and it helps to keep the implant in place. In a small number of patients, however, this capsule of scar tissue tightens, becomes unusually hard and starts to contract around the implant and in severe cases distort the shape of the breast and even cause pain. This is called Capsular Contracture. As the capsule starts to contract around the soft implant, the breast implant starts to feel firm and gradually looks rounder, usually becomes pulled upward.
Once the breast implant is in place, as normal part of the healing process, the body forms a tissue capsule (aka barrier of scar tissue) around the implant. The body forms a capsule like this around any object it recognises as foreign as a protective measure. The tissue capsule around the implant is usually soft or slightly firm but not noticeable, and it helps to keep the implant in place. In a small number of patients, however, this capsule of scar tissue tightens, becomes unusually hard and starts to contract around the implant and in severe cases distort the shape of the breast and even cause pain. This is called Capsular Contracture. As the capsule starts to contract around the soft implant, the breast implant starts to feel firm and gradually looks rounder, usually becomes pulled upward.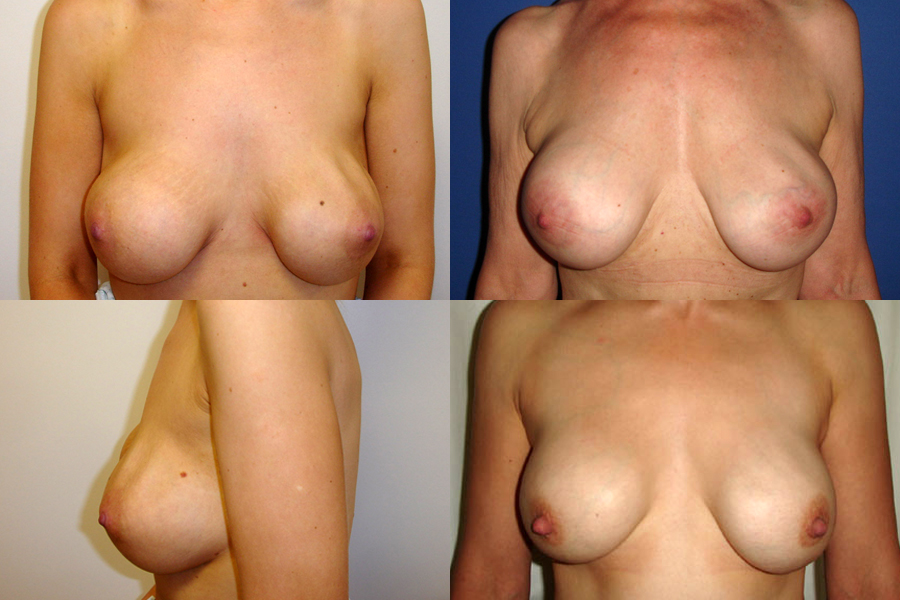 Sometimes following a breast implant surgery, patients may feel and see the wrinkles and rippling (folds) of the breast implants under their skin which may feel uncomfortable and gives the breasts an unnatural appearance. Unfortunately, this may be inevitable, especially following pregnancy or significant weight fluctuations as wrinkling and rippling occurs when the breast tissue is stretched, the implant pocket is enlarged and there isn’t enough breast tissue between the implants and the skin.
Sometimes following a breast implant surgery, patients may feel and see the wrinkles and rippling (folds) of the breast implants under their skin which may feel uncomfortable and gives the breasts an unnatural appearance. Unfortunately, this may be inevitable, especially following pregnancy or significant weight fluctuations as wrinkling and rippling occurs when the breast tissue is stretched, the implant pocket is enlarged and there isn’t enough breast tissue between the implants and the skin.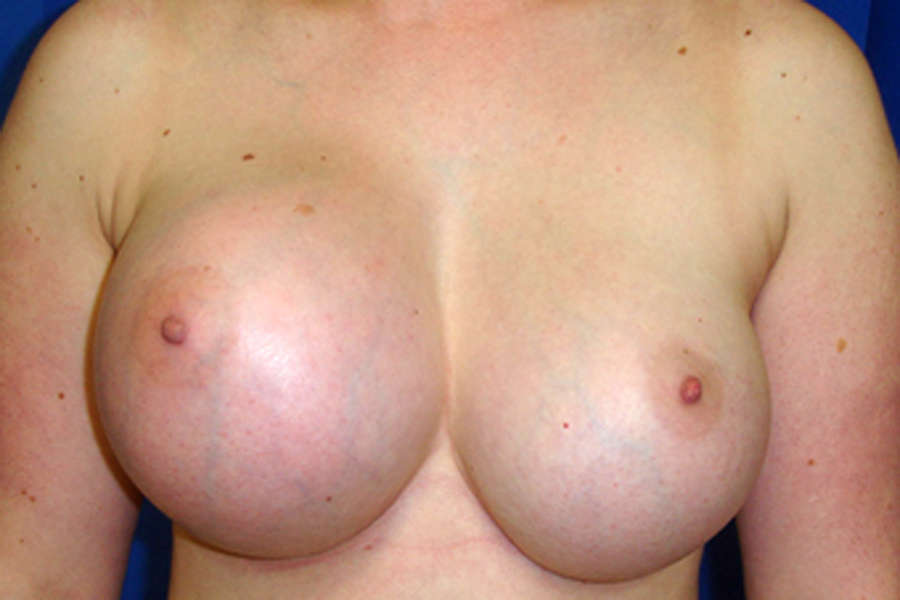 Breast implants are not life-time devices and need to be replaced at some point in time, regardless of the type or brand of the implants. Some manufacturers state a time limit on the lifespan of their implants, whereas others provide lifetime warranty. None of these statements confirm how long the implants really last. In some patients, implants may rupture within the first few years of the implantation whereas for others their implants may last much longer without experiencing any issues.
Breast implants are not life-time devices and need to be replaced at some point in time, regardless of the type or brand of the implants. Some manufacturers state a time limit on the lifespan of their implants, whereas others provide lifetime warranty. None of these statements confirm how long the implants really last. In some patients, implants may rupture within the first few years of the implantation whereas for others their implants may last much longer without experiencing any issues.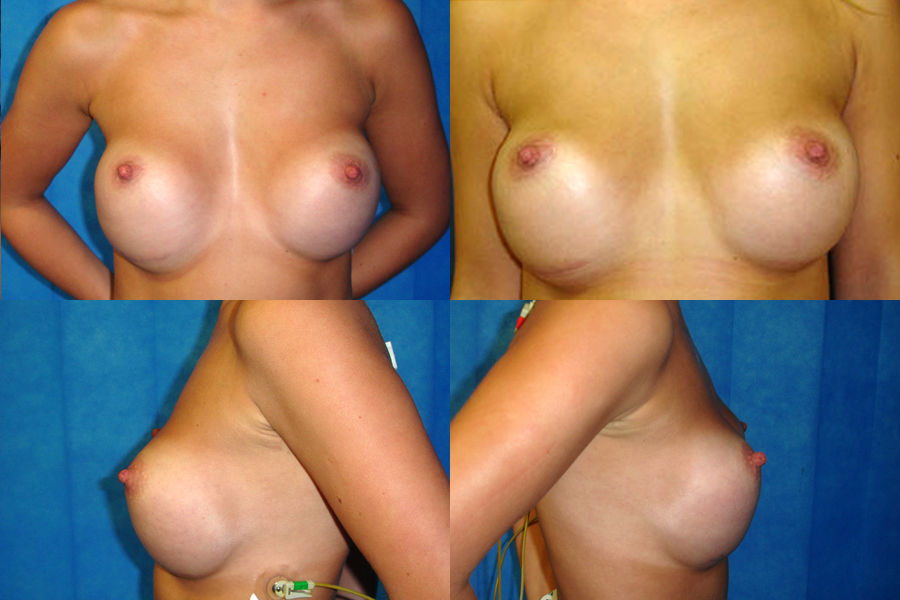 Bottoming out is a complication that occurs when there there’s no adequate support and implant slides too low in the breast tissue, increasing the distance between the nipple and the breast fold. From the front, the nipple appears to be too high on the breast. If looked from the side, the nipple appears to be pointing upwards due to the increased distance between it and the breast fold.
Bottoming out is a complication that occurs when there there’s no adequate support and implant slides too low in the breast tissue, increasing the distance between the nipple and the breast fold. From the front, the nipple appears to be too high on the breast. If looked from the side, the nipple appears to be pointing upwards due to the increased distance between it and the breast fold.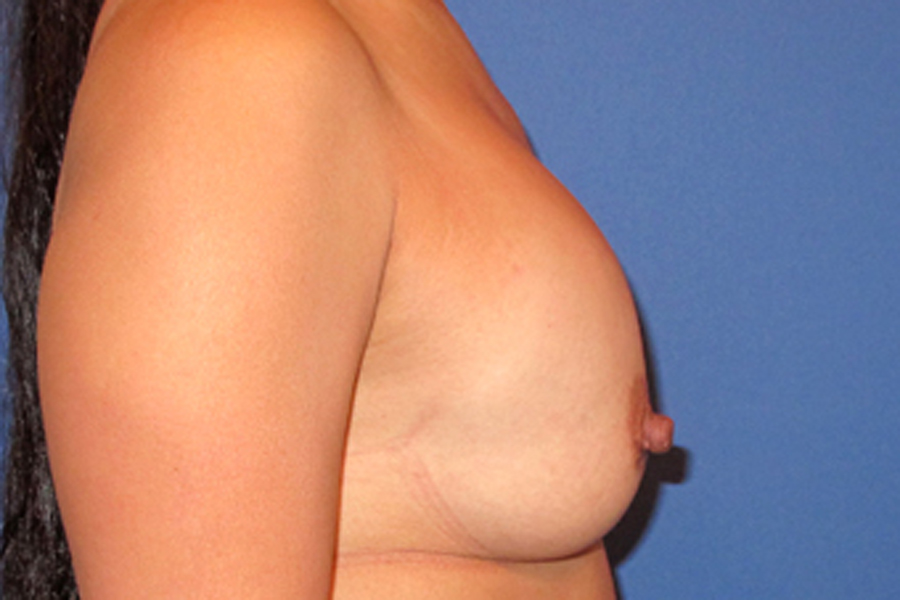 Following Breast augmentation, implants may appear to be sitting slightly too high and to have too much fullness in the upper half, especially when implants are placed sub-muscular or dual plane. This is completely normal, and It takes time for the muscle and tissue to relax and allow the implants to settle in place. The healing period and the settling of breast implants, varies between individuals and is determined by their chest anatomy.
Following Breast augmentation, implants may appear to be sitting slightly too high and to have too much fullness in the upper half, especially when implants are placed sub-muscular or dual plane. This is completely normal, and It takes time for the muscle and tissue to relax and allow the implants to settle in place. The healing period and the settling of breast implants, varies between individuals and is determined by their chest anatomy.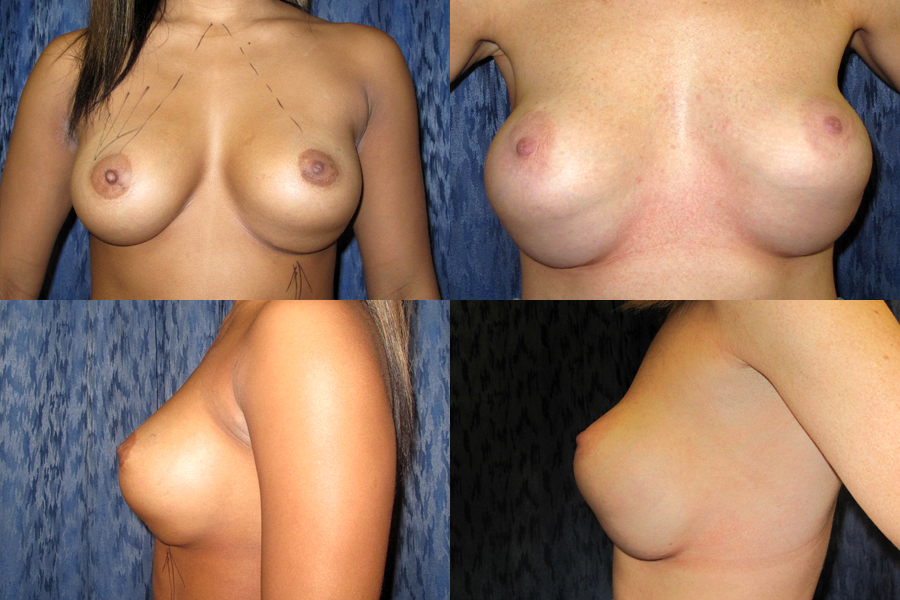 “Double bubble” occurs when an implant or natural breast tissue drops down below the breast fold (inframammary crease), creating an unnatural indentation or line across the lower pole of the breast; causing the appearance of two breasts, from the profile. This condition is more visible when the arms are lifted above the head. Fortunately, double bubble is a relatively rare complication which may occur at any time after breast augmentation surgery and it is treatable in most cases.
“Double bubble” occurs when an implant or natural breast tissue drops down below the breast fold (inframammary crease), creating an unnatural indentation or line across the lower pole of the breast; causing the appearance of two breasts, from the profile. This condition is more visible when the arms are lifted above the head. Fortunately, double bubble is a relatively rare complication which may occur at any time after breast augmentation surgery and it is treatable in most cases.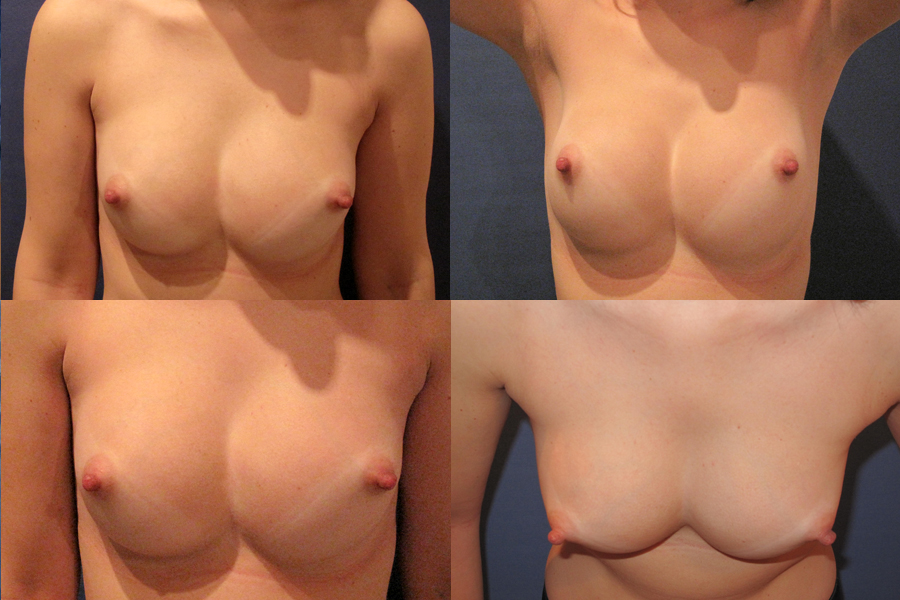 Symmastia also known as “uniboob” is a relatively rare implant complication that occurs when the skin and muscle between the breasts over the sternum (breastbone) detaches and the two pockets of tissue that hold the breast implants come together to form one pocket. This causes one or both implants to shift toward each another, creating the appearance of a single large breast.
Symmastia also known as “uniboob” is a relatively rare implant complication that occurs when the skin and muscle between the breasts over the sternum (breastbone) detaches and the two pockets of tissue that hold the breast implants come together to form one pocket. This causes one or both implants to shift toward each another, creating the appearance of a single large breast.




