(Breast Hardening)
Capsular Contracture or hardening is a breast implant related complication. The body forms a tissue capsules (scar tissue) around every breast implant, it is the body’s natural response to the placement of any foreign object as a protective measure. This capsule is normally soft and unnoticeable. It is only when that tissue capsule tightens/contracts and restricts the movement of the implant that the breast may develop capsular contracture. It should be noted that the implant itself has not changed or hardened, but the capsule squeezing the implant has caused it to feel as though it has. As a result, the breast may feel painful and hard, and depending on the severity of the contracture, the capsule may also affect the appearance or shape of the breast.
Before & After photos
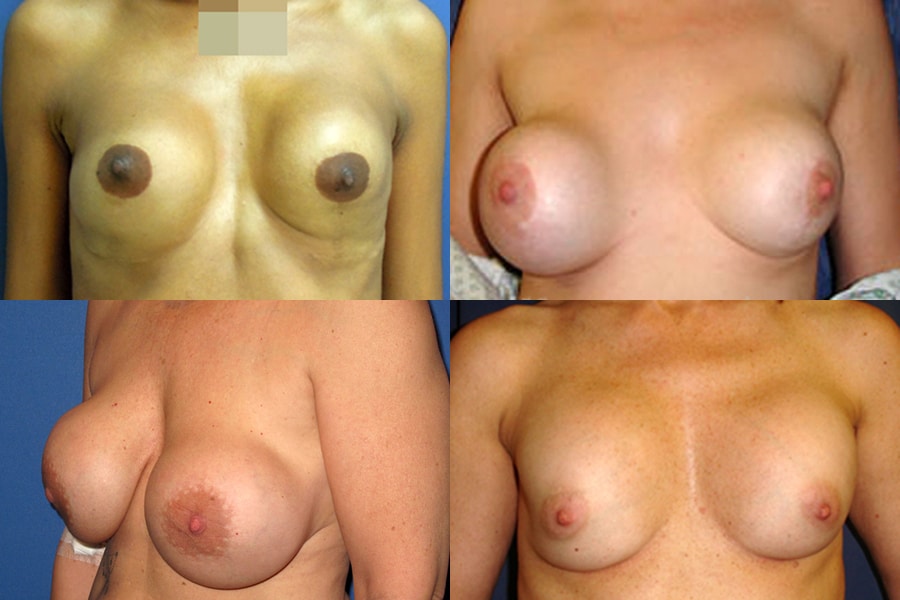
Capsular Contracture or hardening is a breast implant related complication. The body forms a tissue capsules (scar tissue) around every breast implant, it is the body’s natural response to the placement of any foreign object as a protective measure. This capsule is normally soft and unnoticeable. It is only when that tissue capsule tightens/contracts and restricts the movement of the implant that the breast may develop capsular contracture. It should be noted that the implant itself has not changed or hardened, but the capsule squeezing the implant has caused it to feel as though it has. As a result, the breast may feel painful and hard, and depending on the severity of the contracture, the capsule may also affect the appearance or shape of the breast.